Hey, family.
It’s been awhile since I’ve written. Life has been a bit brutal and my plate has been overflowing with responsibilities.
Most of this blog has been dedicated to my skin journey — Topical Steroid Withdrawal. I am now six years into my healing and, sadly, am not fully healed. Especially right now with a bunch of stress surrounding my life, my skin has been playing up. My neck, arms, and hands have been flaring, as well as behind my legs.
If you’d like to learn more about Red Skin Syndrome or Topical Steroid Withdrawal, you can
- Visit ITSAN.org
- Go through this blog’s TSW sections, or
- Watch my documentary — Preventable: Protecting Our Largest Organ
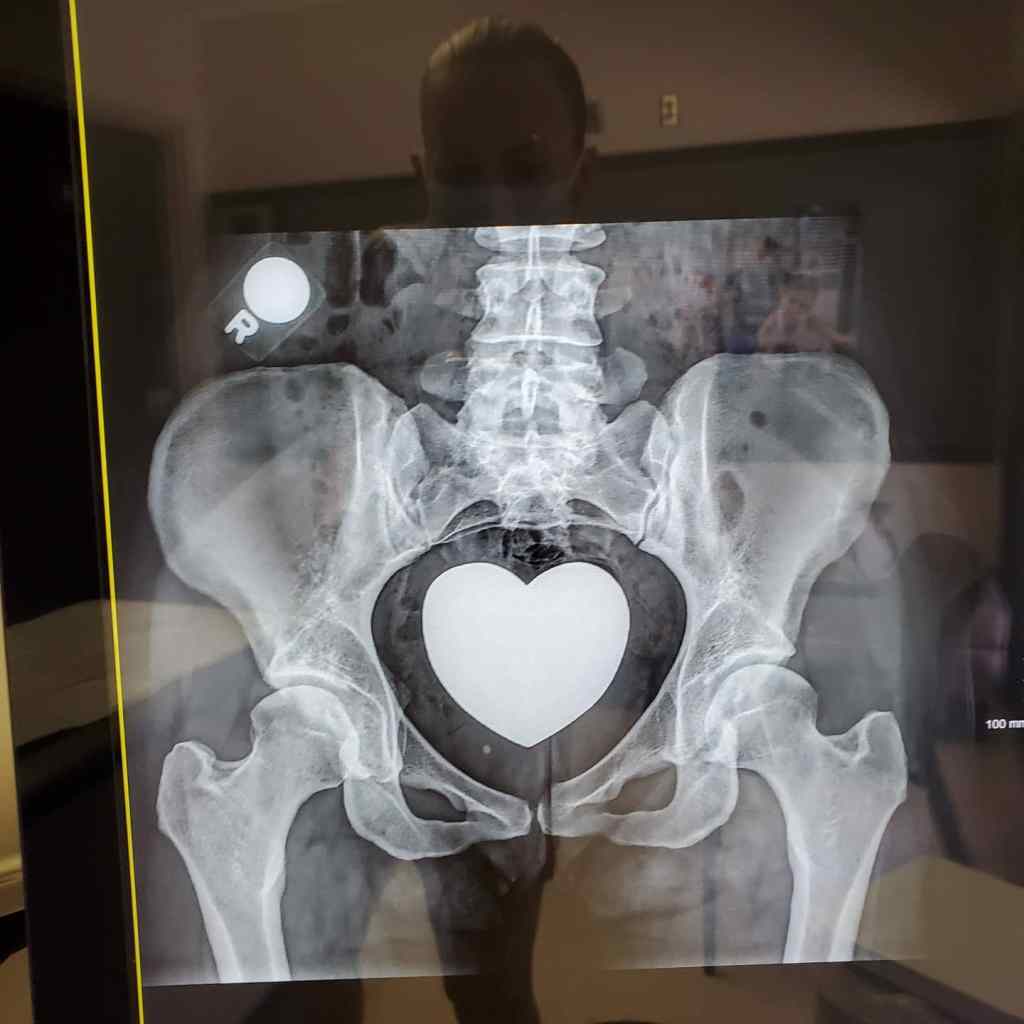
Besides my skin condition, I am now taking on a new recovery. After an MRI and CT scan late 2020, it is seen that I have a tear in my left hip labrum, as well as hip dysplasia — this means I have cartilage damage around my ball joint, and my ball head is not sitting correctly inside the joint. If my ball head isn’t sitting correctly in my joint, it is hitting a spot in the joint that is not meant to take an everyday beating and is most likely the cause for my labral tear. Apparently 80% of patients with labrum issues and hip dysplasia can not fix one problem without addressing the other.
My happy Xray image doesn’t show too much to the untrained eye, but my hip map from my CT shows A LOT. The center edge angle is at 26 degrees, which is right at the cusp of where they would like it to be during surgery. They used to go off of this number for arthroscopy (explained later), and I would have been within the green years ago. But, they started noticing that some people relapsed and would once again damage their labrum. They started looking at other reasons and other angles during surgery consideration — the Tonnis angle and the acetabular coverage. The Tonnis angle shows the roof coverage so to speak of my ball head. For them to do arthroscopic surgery without the PAO (also explained later), I would need to be at 10 degrees or lower. They say 10-12 degrees would be pushing it and that most people in that range end up damaging their labrum again. My number degree… is 17. Yikes! They would NEVER consider surgery for my tear without the PAO. And my acetabular coverage is way under what they would consider as satisfactory. As a dancer, it gives me more flexibility but much less stability.
So, in order to fix the tear, I’ll also need to fix the hip dysplasia. As a dancer, this is devastating news. No dancer wants to take off months to years of work. And on top of the surgical recovery, I am petrified of my skin getting even worse. She is already so angry and flaring, how will she take to TWO massive surgeries?
The first surgery, called arthroscopic surgery, isn’t as invasive as my second surgery, a periacetabular osteotomy. Arthroscopy is known as ‘keyhole’ surgery, where an endoscope is inserted into the joint through small incision(s). Mine will involve three to four incisions. This is to fix my labral tear. It is an outpatient surgery, so no overnight in the hospital will be needed (unless something were to go severely wrong).
The second surgery, a periacetabular osteotomy, or PAO, is simply (in very basic terms) a surgery that would save someone from needing a full hip replacement in the future. Though invasive, that is one piece of news that is music to a dancers’ ears. This is to fix the hip dysplasia. They will cut into my bone and rotate it to a better position, as well as preserve my hip so arthritis doesn’t set in. I will be staying in a hospital for one to two nights after surgery (possibly three if necessary).
Are there risks? Of course. However, allowing more and more degeneration to happen to my hip over the next few decades while also having to endure the pain that comes with degeneration and arthritis, I’d much rather go through a PAO recovery than wait out a hip replacement. I am not a candidate for cortisone shots either (due to my Topical Steroid Withdrawal), so that isn’t even an option in order to help with the pain as the years go on.
Naturally, when I made the final decision to go through this, I immediately took to the internet. I prayed to see stories and blogs of dancers who have done this same surgery and come out on the other side. Thankfully, I did find such blogs, as well as a study!
Study inside the Journal of Hip Preservation Surgery: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5961190/
Other blogs: https://answers.childrenshospital.org/nicole-dancing-through-pain/, https://www.stanfordchildrens.org/en/about/news/releases/2015/sonoma-teen-dancer-realizes-joffrey-dream, https://www.girlfitrocks.com/resources/blog/periacetabular-osteotomy-persevere-and-overcome/, https://web.musc.edu/about/news-center/2020/10/23/dancer-kicking-up-her-heels-after-hip-surgery
Despite some relief while reading these blogs, I didn’t get the full picture of their recovery — just very small highlights. I still have no idea what the extensive recovery physically looks like, the emotional ups and downs that come with recovery, and the hurdles that fall into our recovery path.
This is where I’d like to contribute my piece — to give a more comprehensive look at a dancers recovery from a PAO.
For the first six weeks, I will try and give weekly updates. The first two weeks will be on my arthroscopic surgery, and the following four weeks will be on the PAO recovery. Then, I’ll give bi-weekly updates for another two more months. After that, it’ll be monthly updates until my extra screws get taken out six to ten months after my PAO.
My surgery is in one day. March 10, 2021. Wish me luck!
Bri